The Science of Snoring
Posted on 3/3/23 by Sarah Boudreau
You’ve probably been kept awake at night by the sounds of another person’s snoring — or maybe you’ve been the one keeping other people awake. It’s been estimated that one in four adults snore regularly, and almost half of adults snore on occasion.
Snoring can be an annoyance, but it can also be a symptom of more serious problems, like sleep apnea.
Today on the Visible Body Blog, we’ll talk all about snoring. We promise it won’t put you to sleep!
Snoring: Pathophysiology
The noise behind snoring is caused when the soft tissues around the nasopharynx—typically the soft palate—move due to airflow. The nasopharynx is the upper part of the pharynx that connects to the nasal cavity. Structures like the soft palate, pharyngeal walls, uvula, and tonsillar pillars aren’t supported by cartilage and can vibrate, and that vibration creates noise.
.jpg?width=515&height=386&name=My%20project%20(41).jpg) The pharynx (highlighted in blue). Image from Visible Body Suite.
The pharynx (highlighted in blue). Image from Visible Body Suite.
But if airflow causes the nasopharynx to vibrate, why don’t people snore when they’re awake?
When you fall asleep, your body’s muscle tone decreases. This relaxation can make the airway shrink, limiting airflow. This causes turbulent flow, which is when airflow is irregular and disorganized, and it can make airflow more forceful as the air is pushed through.
When you combine difficult airflow and the soft tissues around the nasopharynx, you get snoring!
Who snores?
There are many factors that contribute to snoring. Here are a few!
- Being a man—men are twice as likely to snore than women
- Sleeping at a high altitude
- Dry or wet air
- Obesity
- Having a low soft palate or large tonsils
- Having a deviated septum or a chronically congested nose
- Old age
- Pregnancy
- Sleeping on your back
Snoring and pathology
Most people who snore experience primary snoring, aka simple or non-apneic snoring. If you have primary snoring, your sleep isn’t disrupted much—even if the noise may bother others. In primary snoring, you don’t wake up in the night due to snoring, your oxygen levels remain normal, and you’re not sleepy during the day.
However, for some, snoring interferes with day-to-day function and is an indicator of a larger problem: sleep-disordered breathing. Sleep-disordered breathing is an umbrella term—a whole range of conditions fall under sleep-disordered breathing.
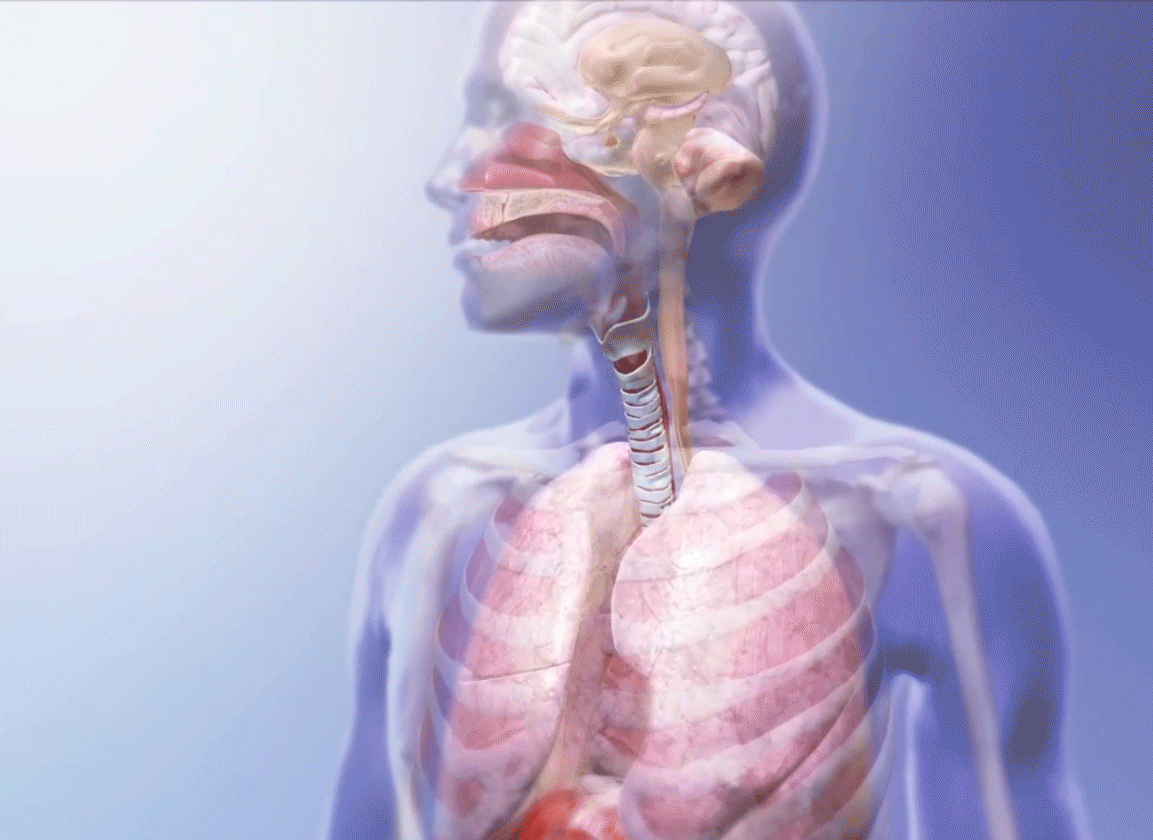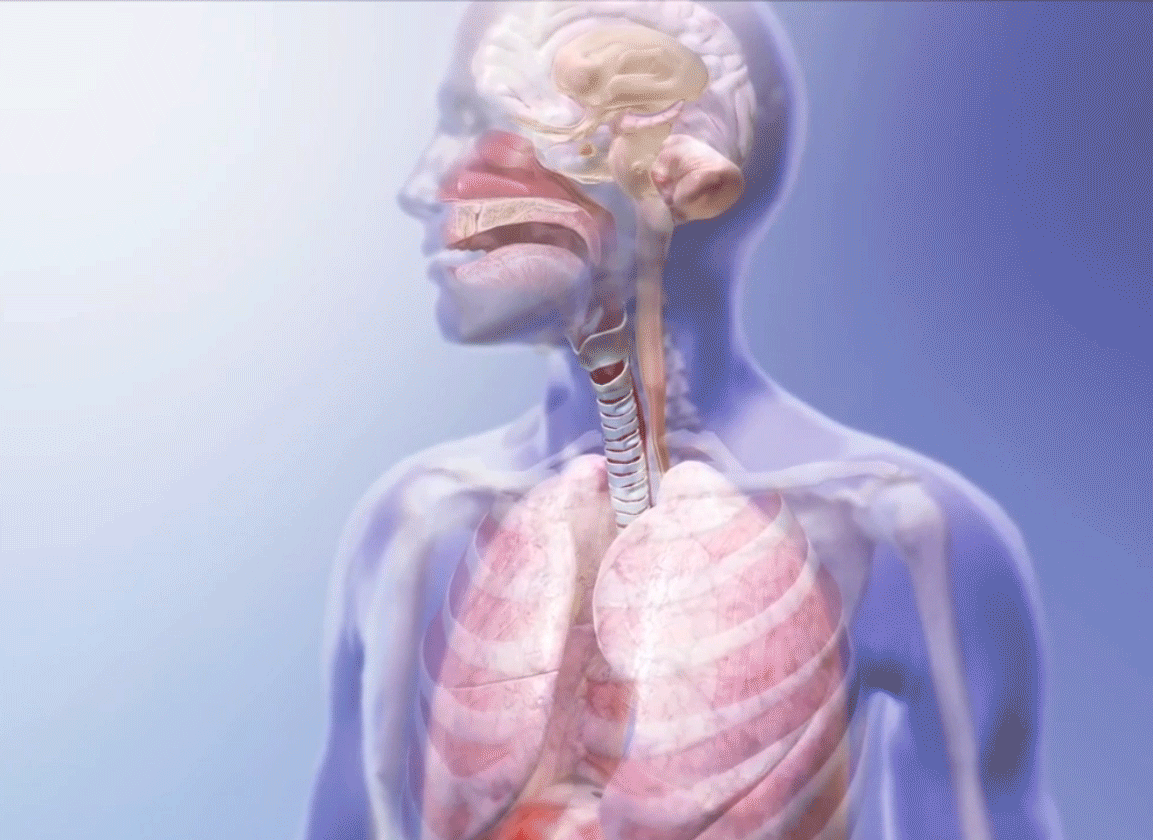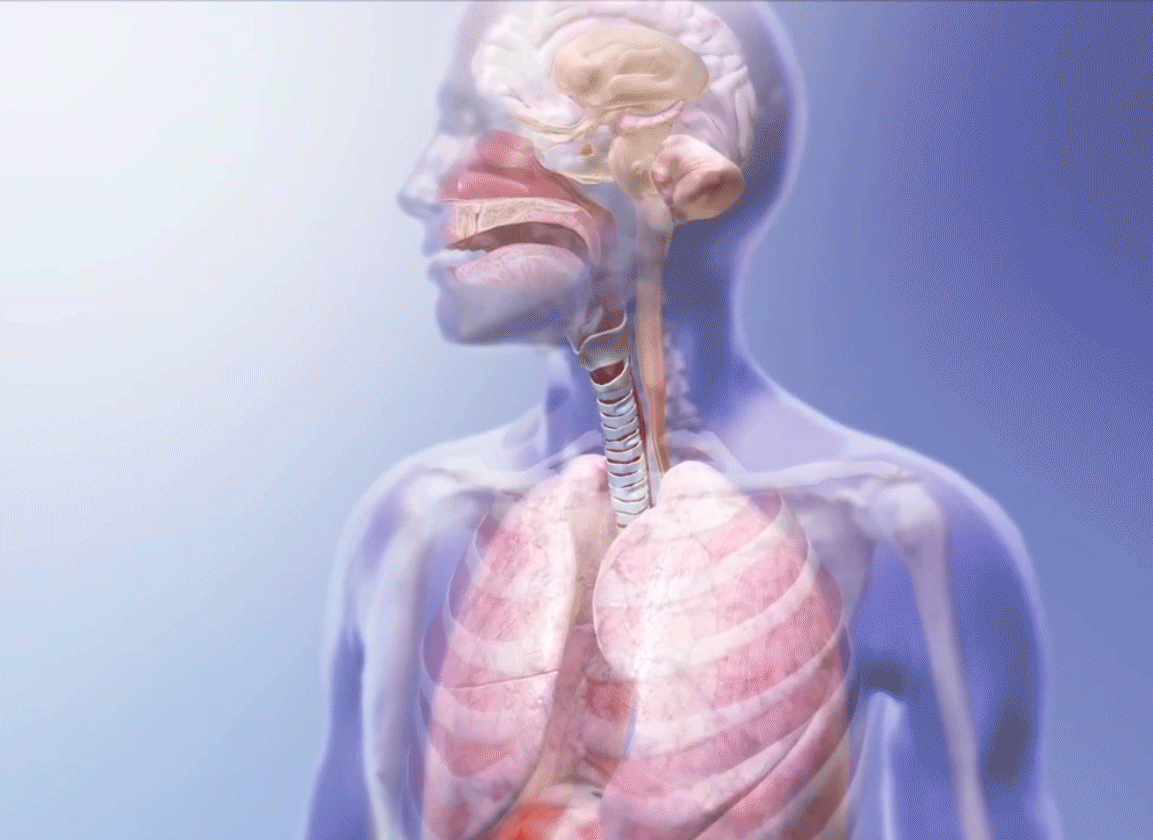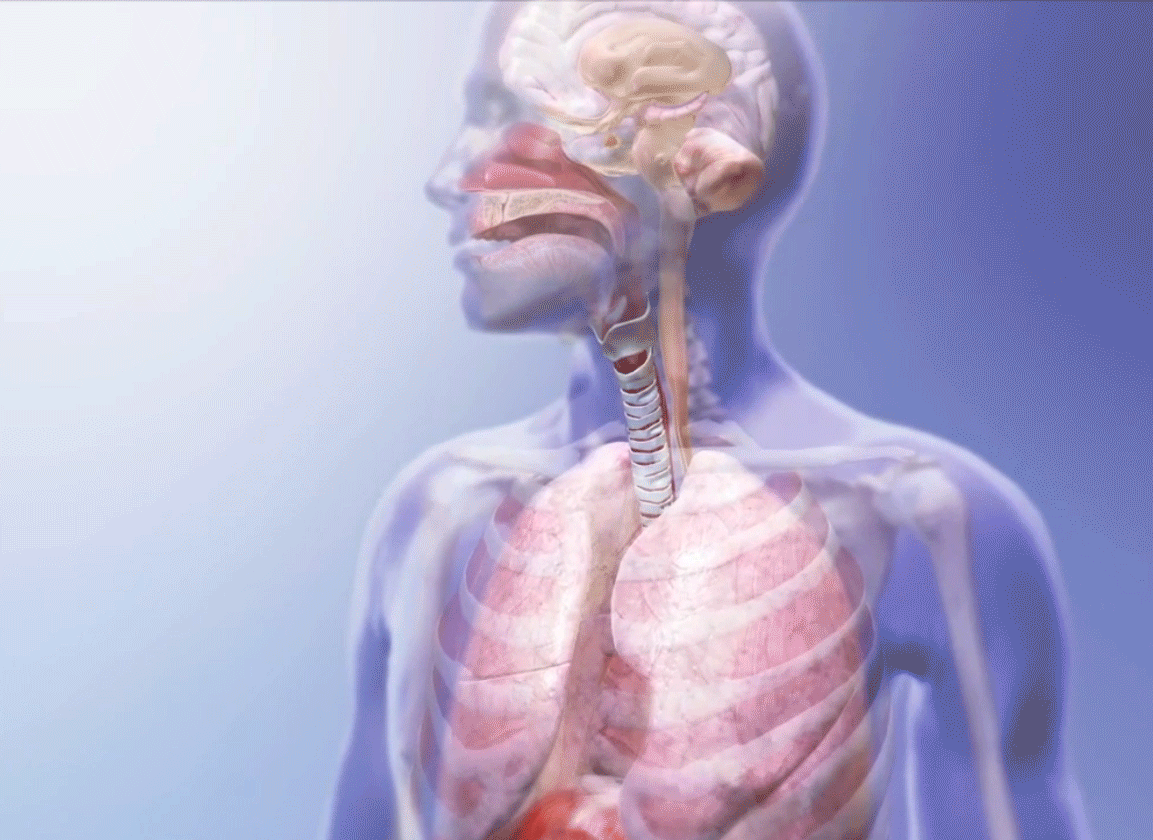 Breathing GIF from Visible Body Suite.
Breathing GIF from Visible Body Suite.
On one side of that spectrum is upper airway resistance syndrome (UARS). UARS occurs when the airway is narrowed and airflow is disturbed, disrupting sleep and causing excessive tiredness during the day. Patients with UARS tend to wake up after two to three hours of sleep.
On the other side of the spectrum is obstructive sleep apnea.
As sleep specialist Lynn A. D’Andrea put it, “Snoring is not an illness, but it is a symptom. Just as a cough can be a symptom of pneumonia, snoring can be a symptom of obstructive sleep apnea.”
Obstructive sleep apnea (OSA) means that during sleep, the airway collapses and air cannot flow in or out of the lungs. Oxygen drops in saturation, and sleep is disrupted, stopping and starting throughout the night. OSA can result in
- Cognitive problems like memory impairment
- Fatigue during the day
- Sexual dysfunction
- Dry or sore throat upon waking
It’s been estimated that OSA affects 2-4% of the population, and it’s considered a risk factor for cardiovascular problems like congestive heart failure and stroke.
Did you know that there’s another type of sleep apnea called central sleep apnea? Central sleep apnea isn’t connected to snoring—it’s when the brainstem doesn’t tell the muscles to inhale during sleep.
Treating snoring
There are several treatment options available for primary snoring; many of them involve devices that open the airways. However, there’s not a lot of research that supports the effectiveness of anti-snoring products, mostly because it’s hard to measure snoring—it’s highly subjective, and the snorer can’t tell what’s working and what isn’t.
 Photo from Campus Productions via Pexels.
Photo from Campus Productions via Pexels.
Common treatment for primary snoring includes devices that hold the tongue in place, mouthpieces that keep the jaw forward to expand the airway, and strips placed on the exterior of the nose that open up the nasal valve. Some people also do special exercises to strengthen their mouths and throats to decrease snoring.
Continuous positive airway pressure (CPAP) machines are typically used to treat OSA, but they can be used for primary snoring as well. CPAP machines deliver a constant air pressure through a mask over the nose, which prevents the collapse of the airway. Since CPAP machines are expensive and bulky, they are rarely used by primary snorers.
Other ways to address snoring include weight loss and cutting down on alcohol consumption before bed. Central fat distribution (fat around the chest and midriff) can push on the diaphragm, decreasing lung capacity, and fat around the throat can put more pressure on the windpipe. Drinking alcohol can make snoring worse by relaxing the throat muscles more.
Changing your sleeping position can also help. Keeping the head propped up with pillows or sleeping on your side are probably the easiest ways to address snoring.
Read More
Learn more about the human body on Visible Body’s blog and Learn Site! Check out these posts:
- Respiratory System Pathologies: Common Diseases and Disorders (via the Learn Site)
- How Does Caffeine Affect the Body? (via the Visible Body Blog)
- Et Tu, Immune System? 4 Seasonal Allergy Facts (via the Visible Body Blog)
- Frightful Physiology: How Horror Movies Scare Us and Why We Can’t Get Enough (via the Visible Body Blog)
- All About Itching (via the Visible Body Blog)
Be sure to subscribe to the Visible Body Blog for more anatomy awesomeness!
Are you an instructor? We have award-winning 3D products and resources for your anatomy and physiology course! Learn more here.



