The Ins and Outs of Asthma
Posted on 2/17/23 by Sarah Boudreau
Asthma is a big deal: it’s a long-term condition that affects about 262 million people worldwide. It affects both children and adults, and it’s the most common chronic disease among children. TV shows and movies depict asthmatics as nerdy and anxious—but what’s the reality behind asthma?
Today on the Visible Body Blog, let’s look at asthma, its causes, and how it’s treated.
What is asthma?
Put simply, asthma is a condition where inflammation causes the air passages in the lungs to narrow, creating symptoms like coughing, wheezing, shortness of breath, and chest tightness.
To understand asthma, let’s first look at the mechanisms behind breathing itself.
When you take a breath, muscles around the lungs create negative pressure, and air comes in through your nose and trachea to relieve that pressure. From the trachea, air moves into the lungs.
Each lung contains a respiratory tree that consists of the bronchi and its subdivisions: the primary bronchi branches into the secondary bronchi, which branch into tertiary bronchi, which then branch into bronchioles.
.jpg?width=515&height=343&name=My%20project%20(39).jpg)
Bronchi branches (left). Image from Human Anatomy Atlas.
Bronchioles are the smallest airways in your body. They contain alveoli, tiny air sacs in the lungs that are encased within capillary networks. The alveoli are where gas exchange happens, which is the process where oxygen moves from the lungs into the blood and carbon dioxide moves from the blood to the lungs.
During an asthma attack, inflammation makes the bronchi more narrow and mucus is secreted, making it more difficult for air to move in and out of the lungs. Asthma is also characterized by bronchial hyperresponsiveness—basically, the airways are very sensitive to triggers.
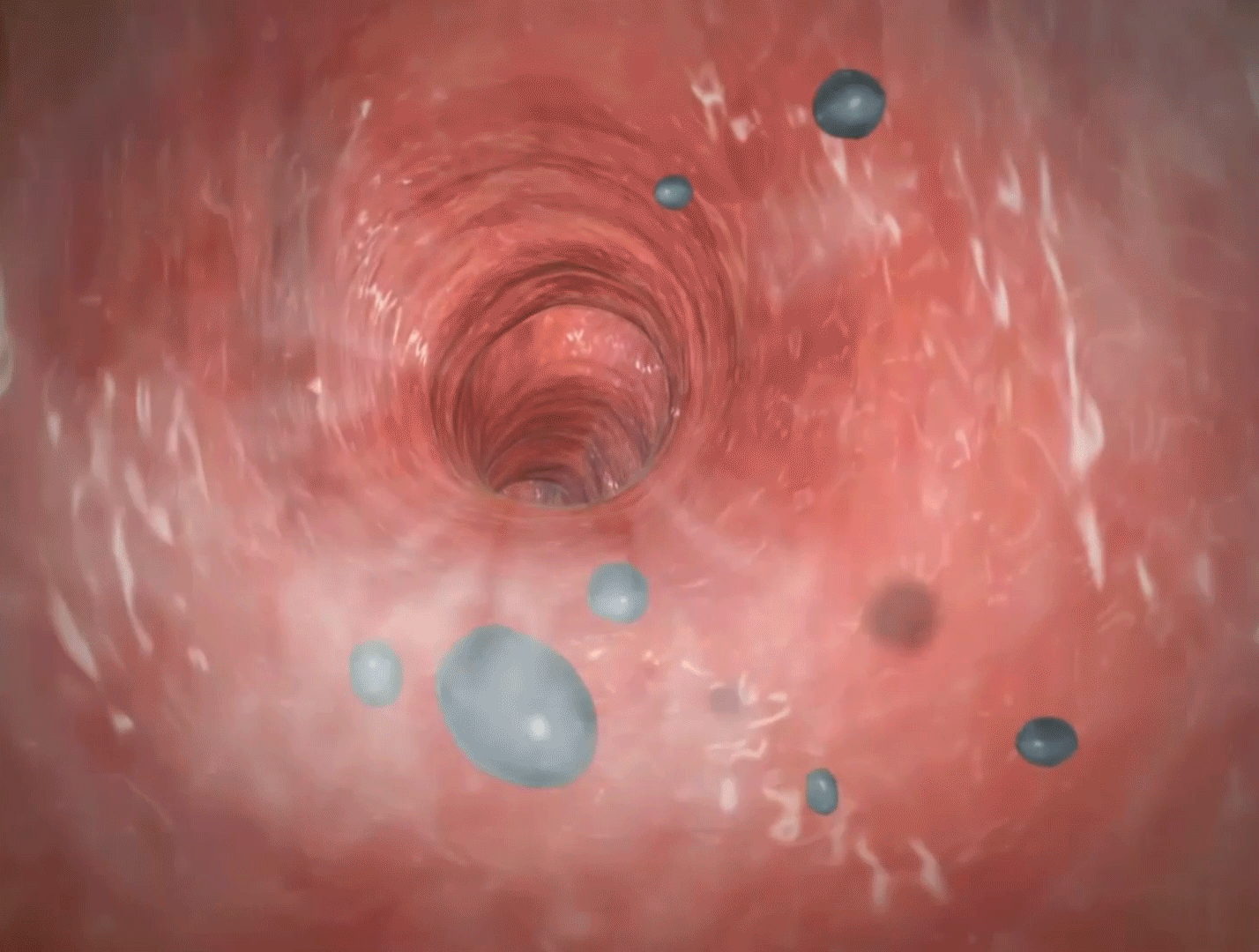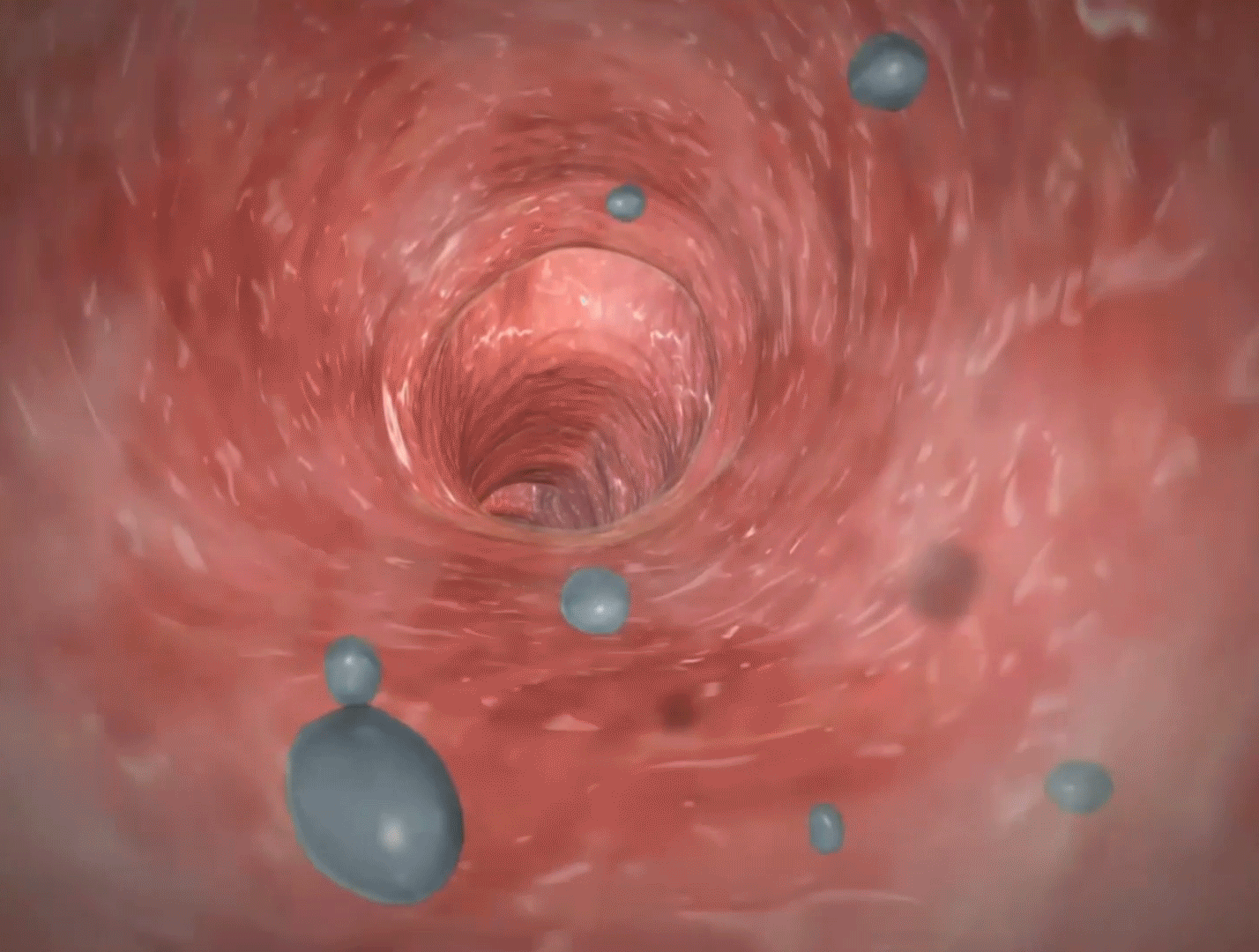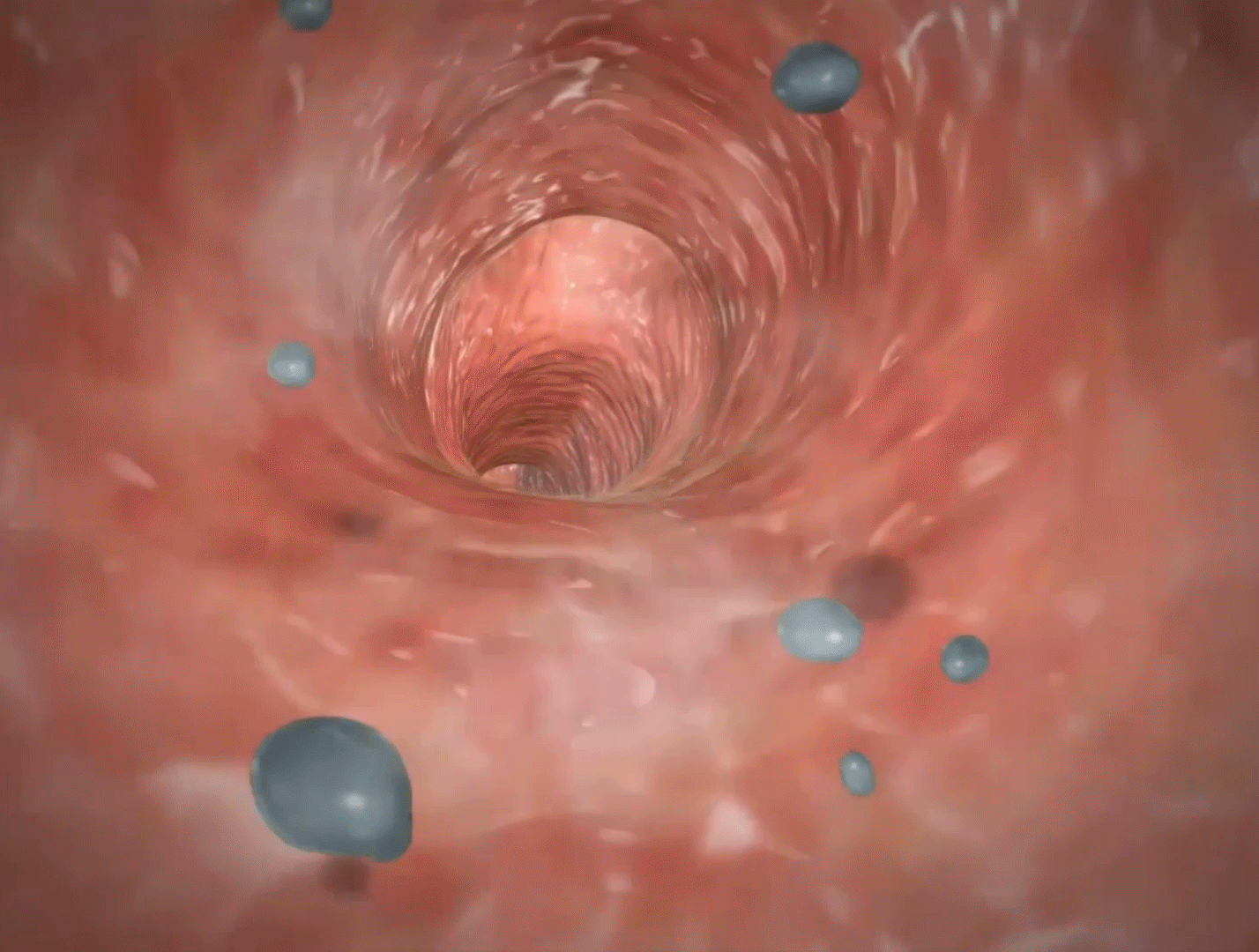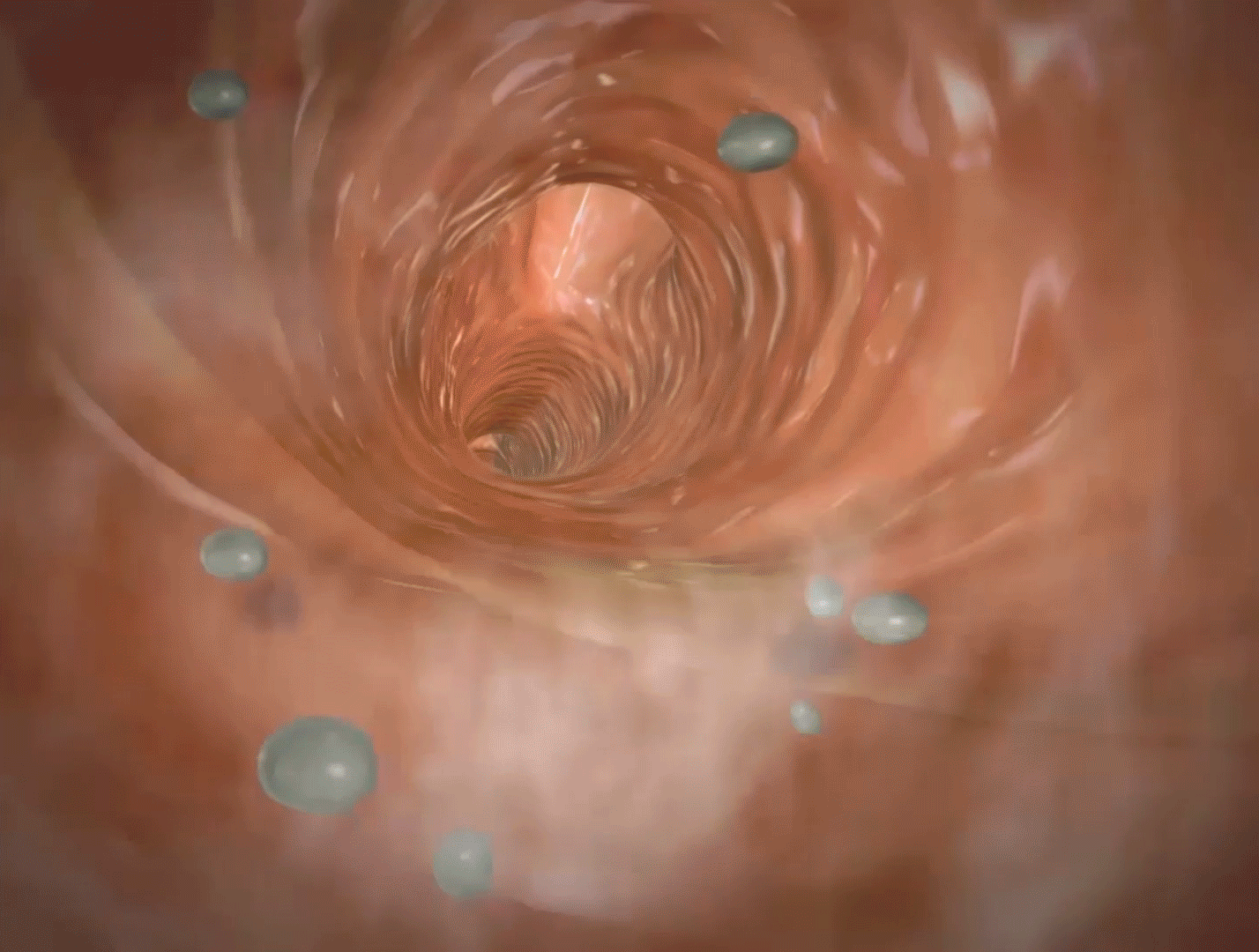
The bronchi narrow and extra mucus is secreted. GIF from asthma animation in Physiology & Pathology, part of Visible Body Suite.
Some triggers for asthma attacks include:
- Irritants
- Infection
- Exercise
- Cold
Now that we’ve covered the basics, let’s dive into more detail! There are actually two phases to an asthma reaction.
In the early phase, the immune system reacts by producing antibodies like IgE, aka immunoglobulin E. When IgE antibodies are released, they are programmed to respond to environmental triggers, like allergens. IgE then binds to mast cells, which are specialized cells that trigger inflammation. When something gets inhaled and triggers mast cells, they release chemicals that contract the smooth muscle of the bronchi.
The early phase of asthma happens in response to a trigger, but the late phase occurs around 4-8 hours later. The early phase sounds the alarm, and several types of white blood cells begin to make their way to the lungs. When they finally arrive, the late phase of asthma begins. These cells create more inflammation and constrict the bronchi. During the late phase, the immune system is even more sensitive to triggers, which can make the asthma attack last even longer.
Some people who struggle with asthma experience airway remodeling, wherein the airways have changed structure and make breathing permanently difficult. One factor that contributes to airway remodeling is bronchoconstriction—when the bronchi are inflamed, more pressure is put on the epithelial cells that cover the inside surface of the bronchi. The extra pressure increases gene expression for epithelial cell genes responsible for growth, forming new blood vessels (angiogenesis), and for creating smooth muscle cells.
What causes asthma?
We’re not exactly sure what causes asthma! Asthma is probably caused by a combination of environmental, genetic, and nutritional factors. There are several factors that increase one’s risk of asthma, including:
- Exposure to household allergens
- Diets low in omega-3 fatty acids and vitamins C and E
- Having a parent with asthma
- Having allergic conditions like eczema or hay fever
- Smoking
- Exposure to pollution
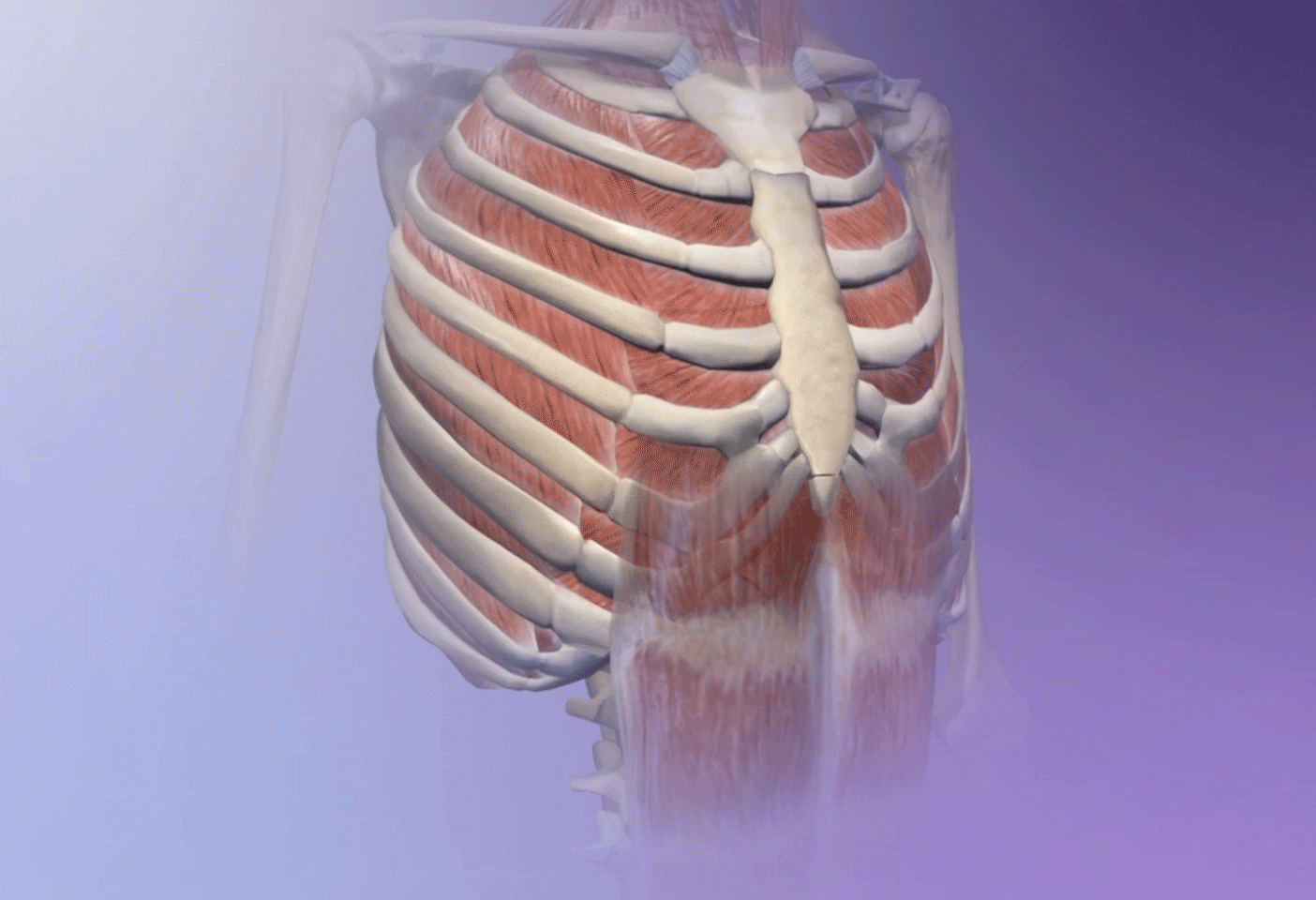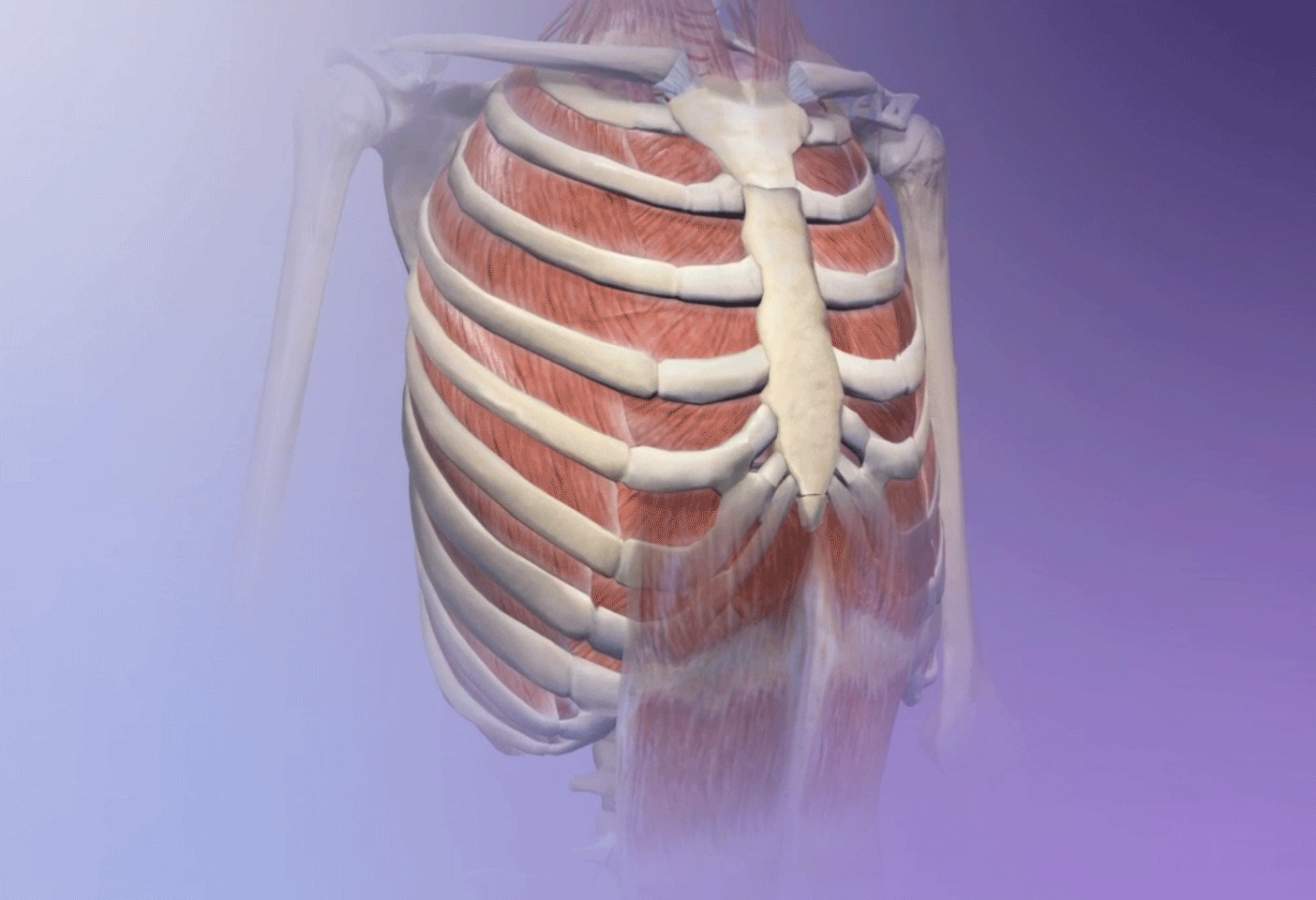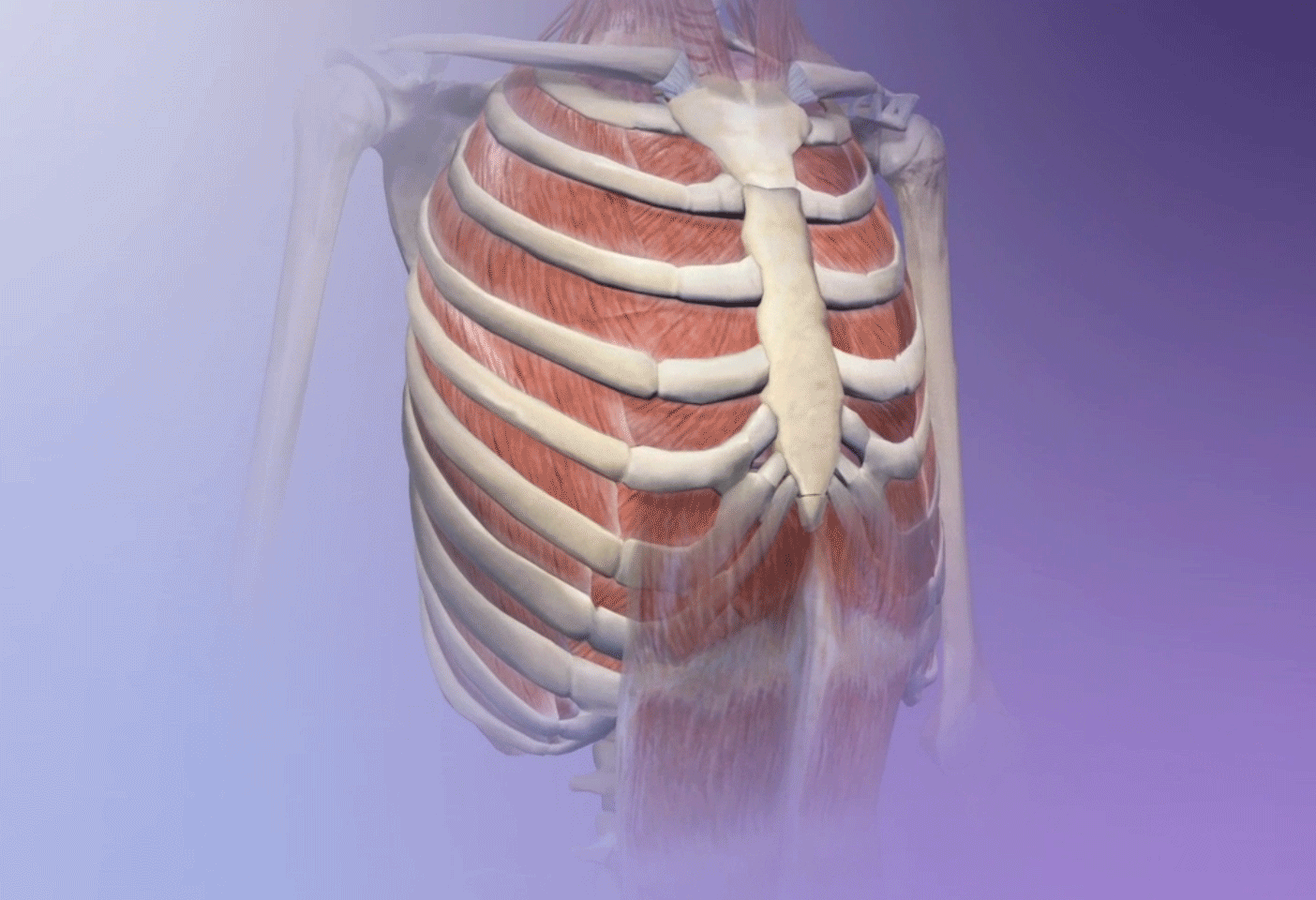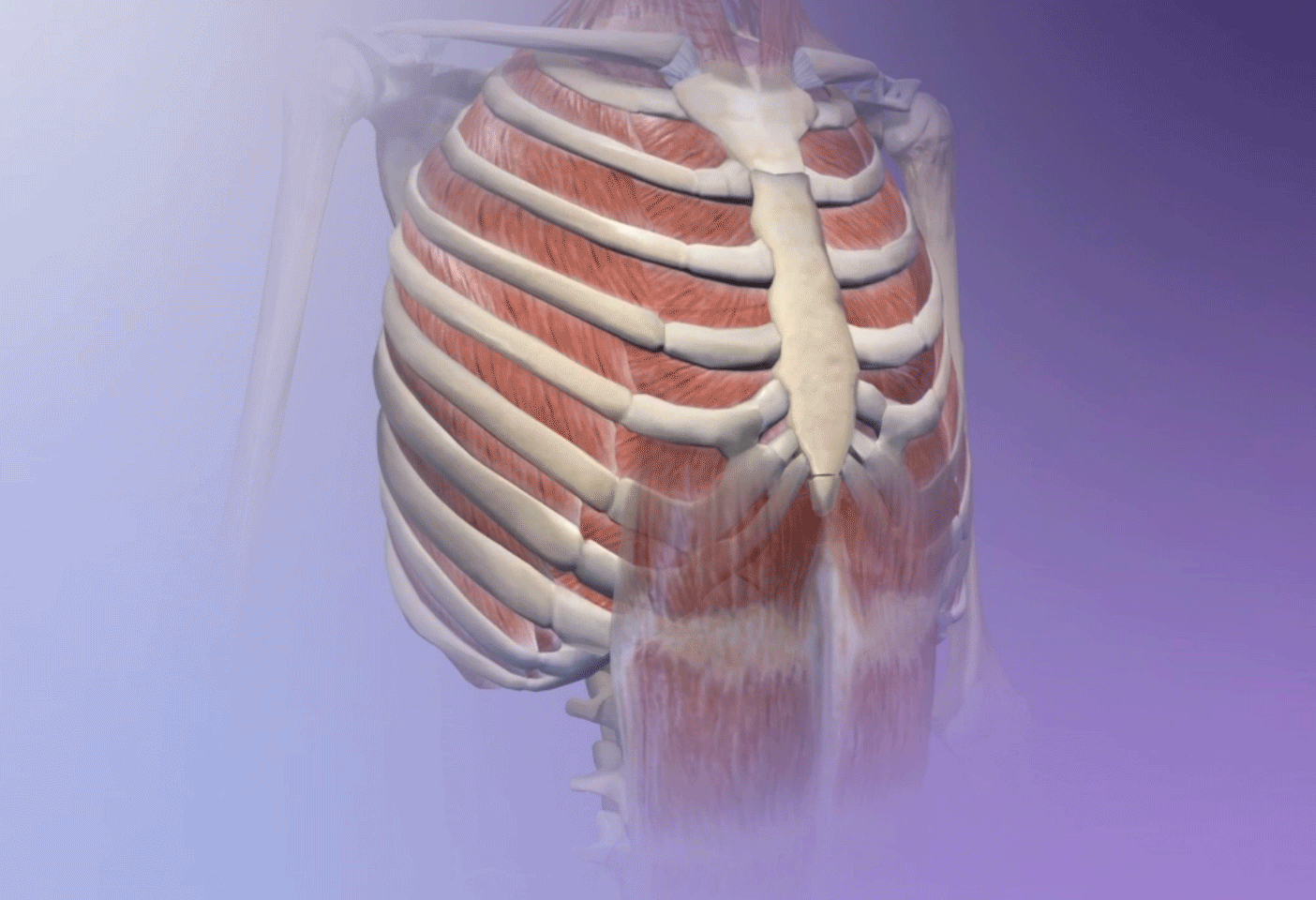
Forced breathing from exercise can trigger asthma. GIF from breathing animation in Human Anatomy Atlas.
Diagnosing asthma
To determine if a patient has asthma, a doctor will ask about medical history and perform lung function tests.
The most common lung function test is spirometry, a test that measures how much air can be inhaled and exhaled. A spirometer is a mouthpiece that attaches to a spirometry machine that measures breaths. The patient is asked to place their lips around the mouthpiece and take the deepest breath they can and exhale as hard as they can. This is done three or more times to get an accurate result. Sometimes, the patient will be given an asthma drug and then will try the spirometry test again to see if the results change. If the lungs become stronger after taking the asthma drug, it’s likely that the patient has asthma.
On the other hand, doctors will sometimes introduce potential asthma triggers and repeat the spirometry test to determine if lung function decreases when the patient is exposed to a trigger.
Figuring out what triggers asthma is a different challenge. Allergy testing on the skin can help confirm a specific allergy, but it doesn’t test for exercise, stress, or other triggers. To figure out what triggers asthma, a patient can record when and where they feel symptoms so they can determine a pattern and narrow down the options.
Did you know that 10-20% of asthmatics are allergic to aspirin and other NSAID pain relievers? Taking an NSAID can cause asthma attacks that can be severe or even fatal.
Treating asthma
To treat their asthma, most asthmatics take controller and quick-relief medicine, which are both usually delivered through inhalers. Controller medicine is taken daily to reduce symptoms overall, and quick-relief medicine is used to address asthma attacks when they occur.

An emergency inhaler. Photo by Luci on Pexels.
There are two different classes of drugs used to treat asthma: anti-inflammatory drugs and bronchodilators. You could probably guess by the name, but anti-inflammatory drugs work against the inflammation that narrows the airway. Bronchodilators work to widen the airways.
Some asthmatics use a peak flow meter to monitor their asthma. Similar to the spirometer, a peak flow meter measures the fastest rate you can push air from your lungs as you exhale. Monitoring this rate can help identify when asthma is getting worse or when there’s an increased risk of an attack.
Types of asthma
Asthma can be classified by symptoms or triggers—for example, exercise-induced asthma—or it can be classified by severity.
Here are the four levels of severity:
- Intermittent asthma, where lung function is normal and symptoms occur less than twice a week. Quick-relief medicine is used two or fewer times a month.
- Mild persistent asthma, where you don’t have daily symptoms, and symptoms occur two or more days a week. Quick-relief medicine is used more than twice a week.
- Moderate persistent asthma, where you have symptoms almost every day and are awakened one or more nights a week. Lung function is decreased, and quick-relief medicine is needed more than twice a week.
- Severe persistent asthma, where there is a significant decrease in lung function. Symptoms occur every day, and it wakes you up every night. Quick-relief medicine is needed several times a day.
Conclusion
Asthma is a very common chronic disease where triggers such as allergens or exercise cause inflammation and extra mucus production in the airways, which causes them to narrow. Narrowed airways mean that breathing is more difficult. Asthma can interfere with day-to-day activities, and it’s treated with controller inhalers (which prevent symptoms) and rescue inhalers (which address asthma attacks).
Want to learn more about the respiratory system? Check out these blog posts!
- The Wonderful Windpipe: Five Awesome Facts about the Trachea
- Anatomy and Physiology: The Relationships of the Respiratory System
- Anatomy and Physiology: Gas Exchange
Be sure to subscribe to the Visible Body Blog for more awesomeness!
Are you an instructor? We have award-winning 3D products and resources for your anatomy and physiology or biology course! Learn more here.



