It’s Electric!: The Cardiac Conduction System
Posted on 2/11/22 by Sarah Boudreau
The healthy heart pumps five to six liters of blood every minute—if you’re like me and visualized that as three two-liter soda bottles, you know that’s a lotta liquid. The pumping motion of the heart is a result of electrical impulses that coordinate the contraction of the heart’s chambers. Generated in the heart itself but controlled by the autonomic nervous system, those impulses spread from cell to cell to make the muscles contract. The rhythm of those contractions creates the heartbeat.
Today on the Visible Body blog, we’ll highlight the heart’s conduction system, from the node that creates the first electric impulses to the fibers that deliver those impulses to the chambers. We’ll also talk about sick sinus syndrome, a condition that causes an irregular heartbeat.
If you’re an instructor looking for new ways to teach the conduction system, check out this video!
Sinoatrial node
Known as the SA node for short, the sinoatrial node is nicknamed the pacemaker. The SA node is flat, up to 25 millimeters in length, and is located in the superior posterolateral wall of the right atrium in the subepicardial layer of the heart. It’s made up of pacemaker cells: myocardial cells that are specialized to conduct electrical impulses.
The SA node generates an electrical stimulus 60-100 times per minute, creating the sinus rhythm, which is the normal electrical pattern of the heart.
A pathway called the interatrial bundle carries impulses to the left atrium.
Each impulse spreads throughout the right atrium through internodal pathways. The internodal pathways are made up of anterior, middle, and posterior bands, and they connect the SA node to the atrioventricular (AV) node, located on the upper part of the right atrium. This journey takes about 50 milliseconds.
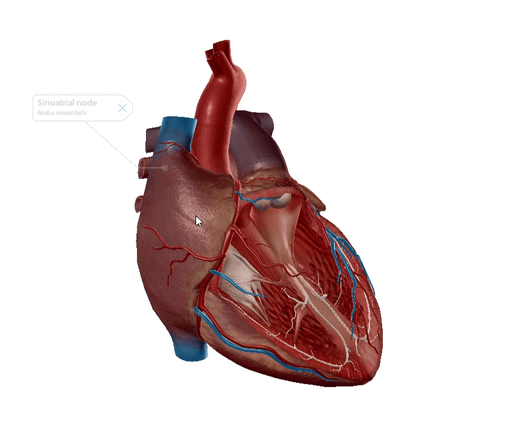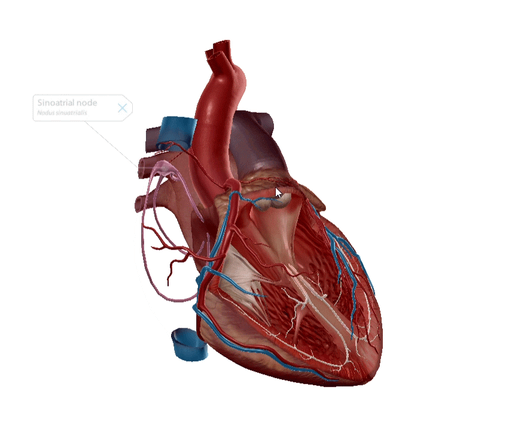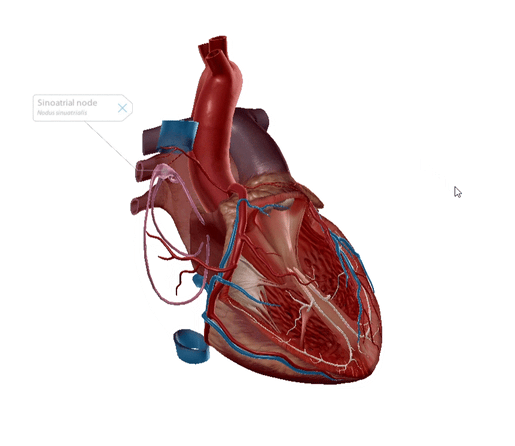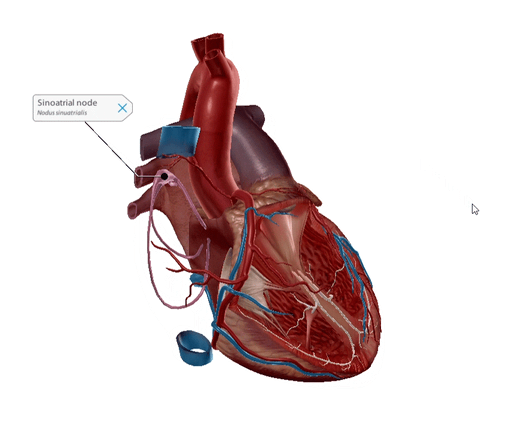 GIF from Human Anatomy Atlas.
GIF from Human Anatomy Atlas.
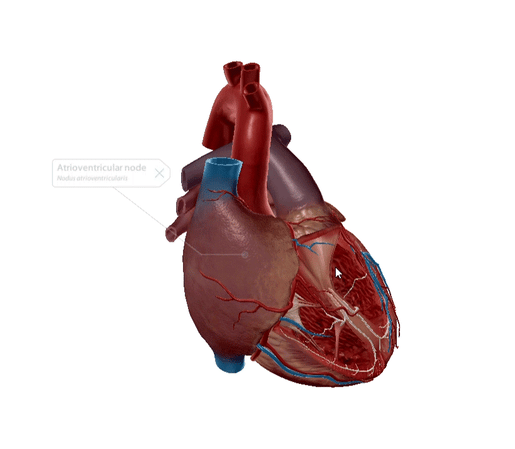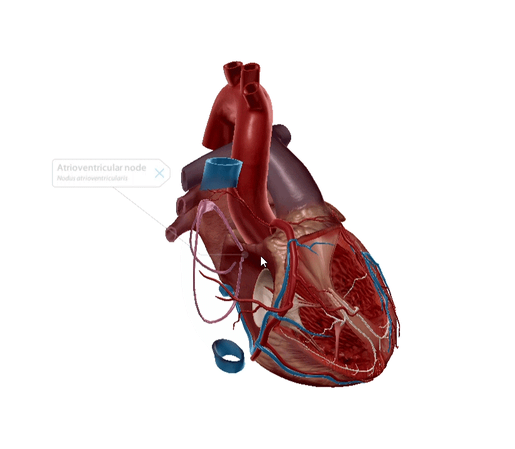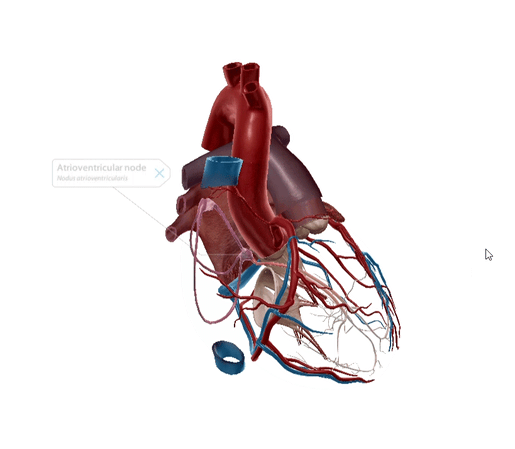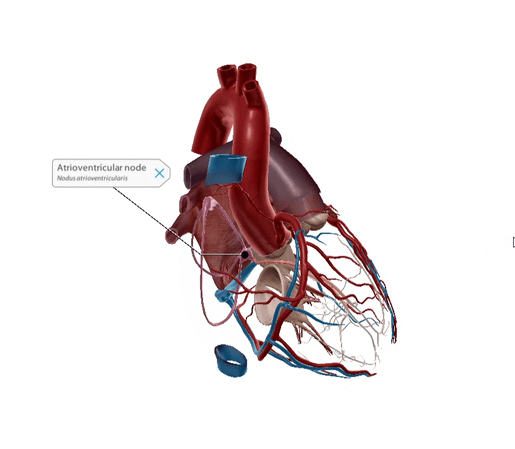
Atrioventricular node
The atrioventricular or AV node is the “secondary pacemaker” of the heart. The main job of this conducting tissue bundle is to act as the middleman, conducting electrical impulses received from the SA node into the bundle of His.
Made up of pacemaker cells and transition cells, the AV node is smaller than the SA node and is located in the posteroinferior part of the interatrial septum.
The AV node creates a slight pause before the electrical impulse is sent down the line. This pause allows the atrial cardiomyocytes to pump blood into the ventricles before the next impulse reaches the ventricles.
The AV node conducts electricity slower the more it is stimulated. This protects against an excessive heart rate if the heart were to beat irregularly.
 GIF from Human Anatomy Atlas.
GIF from Human Anatomy Atlas.
Bundle of His and the left and right bundle branches
Named for Swiss cardiologist Wilhelm His Jr, the bundle of His is made of wide muscle fibers that conduct electrical impulses quickly.
The bundle begins where the AV node enters the central fibrous body of the heart. It consists of three regions:
- The penetrating bundle, which enters the central fibrous body
- The nonbranching bundle, which passes through the central fibrous body
- The branching bundle, which exits the central fibrous body
The branching bundle does what a branching bundle does best: it branches. It branches into the left and right bundles.
The right bundle branch is to the right of the septum and branches into the right ventricular walls and on to the right side of the ventricular apex, where it then enters the septomarginal moderator band and reaches the right anterior papillary muscles. The right bundle branch is responsible for delivering the electrical impulse to the right ventricle.
The left bundle branch is bigger than the right—the left side of the heart is bigger, so this makes sense. It consists of two fibers: one anterior and one posterior. Similar to its right bundle cousin, the left bundle branch moves along the left side of the septum and delivers the electrical impulse to the left ventricle.
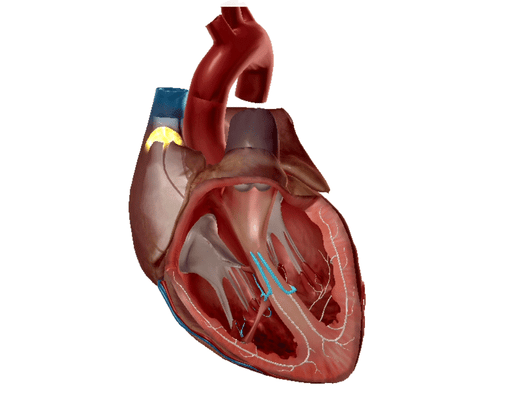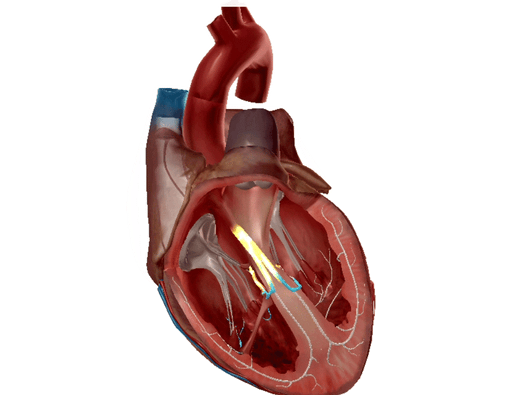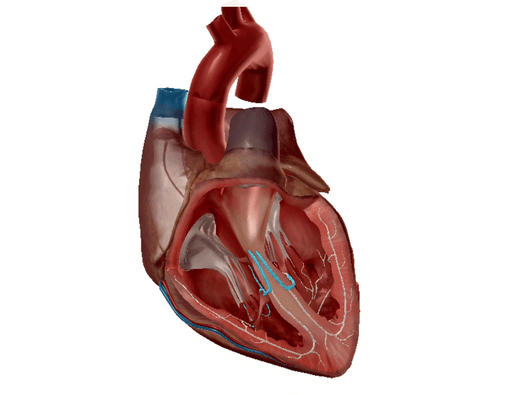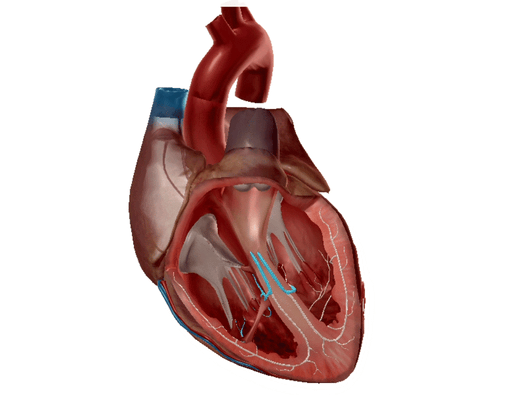
Left and right bundle branches highlighted. GIF from Physiology and Pathology.
Purkinje fibers
Purkinje fibers are conductive fibers located in the muscular ventricular walls. Purkinje cells are larger than myocardial cells and have a higher conduction velocity, with fewer myofibrils and higher glycogen levels. The fibers have more gap junctions, which are channels that connect adjacent cells. This makes Purkinje fibers conduct electricity 150 times faster than AV nodal fibers.
Purkinje fibers start at the apex and spread towards the atrioventricular septum on both sides. Therefore, the electrical impulse starts at the apex and moves to the base of the heart, and the corresponding muscles squeeze, starting at the apex, and pump the blood into the aorta and pulmonary trunk.
Does the name Purkinje sound familiar to you? In addition to discovering Purkinje fibers, the nineteenth century Czech anatomist and physiologist Johann Evangelist Purkinje (also called Jan Evangelista Purkyně) discovered Purkinje cells, some of the largest neurons in the human brain; the Purkinje effect, which is the human eye’s reduced sensitivity to dim red light in comparison to dim blue light; Purkinje images, which are reflections of light off of the human eye; and the Purkinje shift, which is when reds appear darker to the human eye as light levels decrease. On top of all that, he also coined the terms plasma and protoplasm. Busy guy!
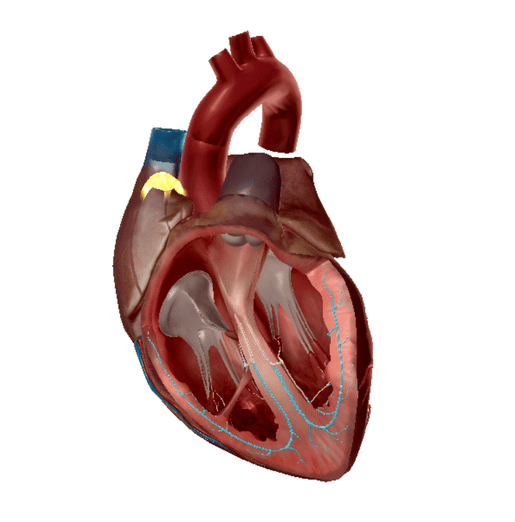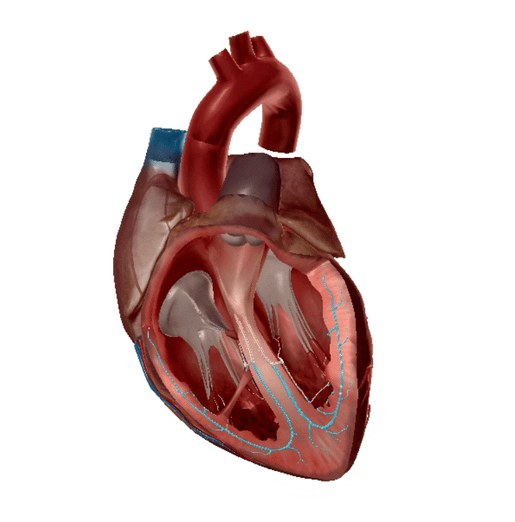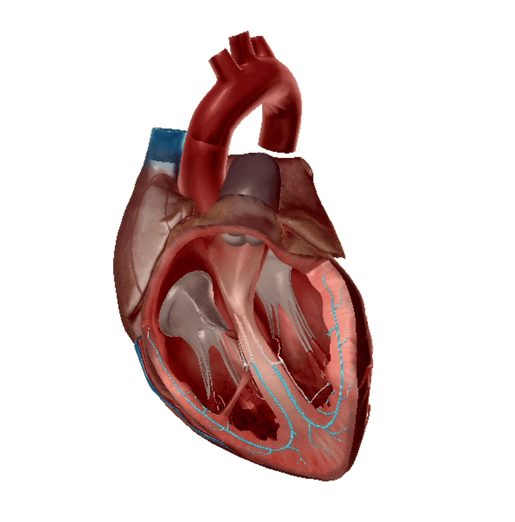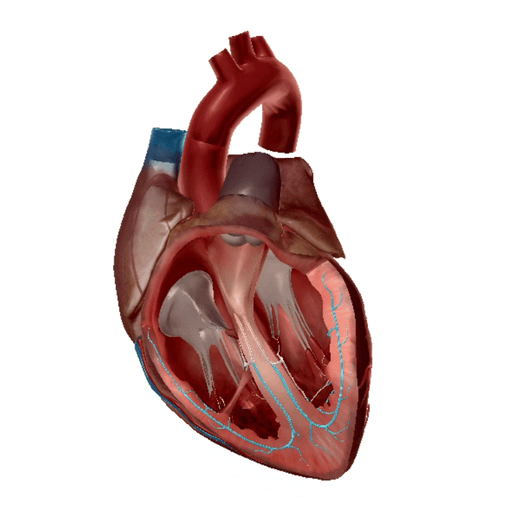
Purkinje fibers highlighted. GIF from Physiology and Pathology.
Sick sinus syndrome
Sick sinus syndrome (SSS) occurs when the SA node becomes damaged. SSS describes heart rhythm problems such as if the heartbeat stops (sinus pauses or sinus arrest), if the heartbeat alternates between slow and fast rhythms (bradycardia-tachycardia), or if the heartbeat is too slow (sinus bradycardia),
SSS is the most common reason that people need an artificial pacemaker. Sinus bradycardia is the most common type of sick sinus syndrome, and over 50% of sick sinus syndrome patients develop bradycardia-tachycardia.
SSS affects men and women at equal rates, and it usually occurs in adults over 70, but can occur in children, usually because of heart surgery that has damaged the SA node.
The cause of SSS is not fully understood, but we do know that certain medications like digitalis, calcium channel blockers, beta-blockers, and anti-arrhythmic drugs can worsen abnormal heart rhythms.
Diagnosis can be made through electrocardiogram in addition to symptoms, which include dizziness, fainting, chest pain, and heart palpitations. Treatment may include changing medications if you are taking one known to cause SSS, taking blood thinners, and getting a pacemaker implant.
A pacemaker implant is not a substitute for the SA node—it’s more of a helpful backup to pick up the slack when the heart doesn’t beat as quickly as it should. A pacemaker is made up of a pulse generator, leads, and an electrode on each lead.
The pulse generator is made up of a battery and a small computer that determines if the heartbeat is lagging. If the heartbeat needs regulation, the pulse generator sends electricity through the leads, which are insulated wires that connect to the heart’s chambers.
The most common method of implanting a pacemaker is transvenous implantation, which usually takes about an hour and only requires local anesthetic. The cardiologist makes a small incision below the collarbone and inserts the leads into a vein. Using X-ray imaging, the leads are guided into the heart and attached. The other ends of the leads are then attached to the pulse generator, which sits between the skin and the chest muscles near the collarbone.
Magnetic fields can interfere with the pacemaker, so people with pacemaker implants should stay away from certain equipment that contain large magnets or can generate a magnetic field. It also means that MRIs are off the table.
Want to read more about the heart? Check out these blog posts!
- Learn Heart Anatomy: Vessels, Valves, and Chambers (oh my!)
- That Boom Boom Pow: Virtual Dissection (sort of) of the Human Heart
- Decoding the Heart: What Is an EKG?
Be sure to subscribe to the Visible Body Blog for more anatomy awesomeness!
Are you an instructor? We have award-winning 3D products and resources for your anatomy and physiology course! Learn more here.



