3 Ways Technology is Helping in the Fight Against COVID-19
Posted on 5/15/20 by Laura Snider
Here at VB, we’ve been reading about COVID-19 in the news almost nonstop as the pandemic continues. Given that we keep a close eye on advancements in medical research and technology, we’ve noticed several ways in which healthcare professionals and researchers have been using technology in innovative ways to diagnose, analyze, and treat this new virus. Here are three we thought were especially interesting!
1. Developing more tests and modeling drug interactions
Here in the US, we have an alarming shortage of testing for COVID-19. Even when patients who potentially have the virus can get tested, analysis of the results of the tests that are our current standard can take several days. The tests we’re currently using involve a clinician taking a sample, usually via a swab that goes up the nose and collects mucus from the nasopharynx, and sending that sample to a lab where specialized equipment is used to analyze the results.
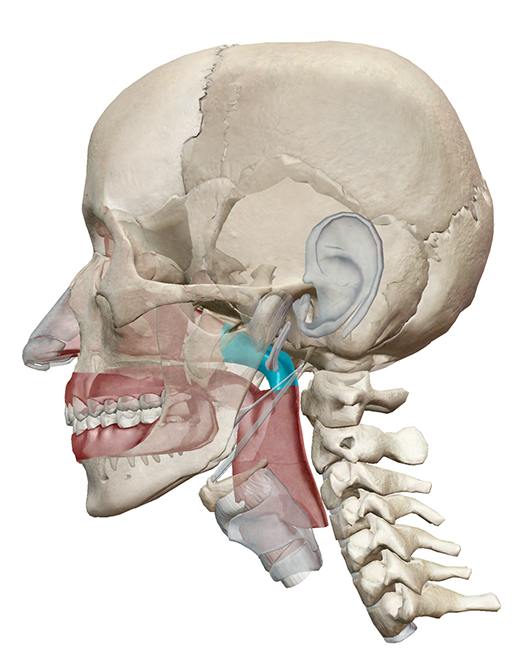
The nasopharynx (highlighted) connects the nasal cavity and the oropharynx, allowing for the passage of air (and mucus). Image from Human Anatomy Atlas.
But researchers have recently been looking at another, quicker way to detect the virus: antigen tests. Whereas a PCR (polymerase chain reaction) test searches for the presence of the virus’ genetic material in a sample, an antigen test looks for specific proteins on the outside of the virus.
Antigen tests also have a few advantages: they’re cheaper to produce, and they yield results much more quickly because they don’t require sending samples out to a lab. Some of the antigen tests currently in development could be carried out by patients at home.
The downside is that antigen tests “could miss around 15-20% of infections”, which means they are significantly less reliable than the PCR tests. A 15% rate of false negatives is nowhere near good—it would mean that some people who actually do have the virus don’t think they’re infected and could continue to spread it to others.
However, given their low cost and quick results, it would be much easier to achieve widespread availability of antigen tests. This means that they have the potential to be useful in screening patients quickly to see if they need further, more detailed testing.
While some teams are working on technology to aid in diagnosis, others are closely studying the structure of SARS-CoV-2 and running simulations to see how the virus interacts with human tissues and how different drugs could be used to interfere with those interactions. They’re also looking closely at a wide range of biological processes that could be exploited using medications to combat the virus.
Tech giants and government agencies have formed a consortium to make supercomputing resources available to researchers working towards COVID-19 treatments. The use of these supercomputers has greatly accelerated the computational modeling work of a group from MIT who are working on a drug that could use a “decoy” version of a protein (ACE2 receptors, which have been a popular target in COVID-19 drug research) that the virus would bind to in lieu of the body’s cells.
Though we might not have thoroughly tested treatments and vaccines for a while yet, there’s no doubt that scientists are doing all they can to find solutions.
2. Using ultrasound to provide rapid point-of-care imaging
Doctors working in emergency medicine often use point-of-care ultrasound to aid in the rapid evaluation of patients, and it looks like they are adapting this technology to help identify signs of COVID-19.
In this Fast Company article, Dr. Resa E. Lewiss describes what she and her colleagues look for in patients they suspect have COVID-19: “We look for an irregularity in the lung lining—it looks more white than normal and less of a crisp straight line on the black-and-white screen. We look for vertical lines that start from the pleura and travel through the lung to the edge of the screen and call these B-lines, a pattern that indicates inflammation or infection in the lung tissue.”
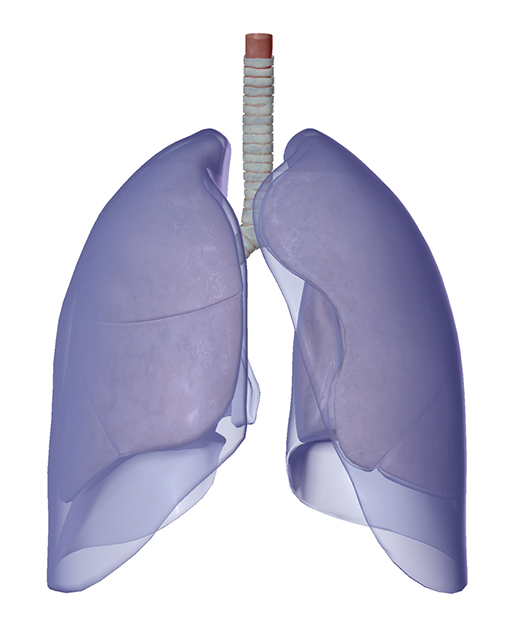
The pleurae. Image from Human Anatomy Atlas.
According to Lewiss, a CT scan will show similar signs of infection, but ultrasound is more quickly and easily administered in an ER environment—the machines used for point-of-care ultrasound are light and portable, and don’t expose the patient to any radiation.
3. Keeping routine healthcare visits going at a distance via telemedicine
We recently talked on the blog about how telemedicine is the next big thing in healthcare, but little did we know at the time of writing that article that, much like remote learning, remote healthcare would be unexpectedly thrown into the spotlight by a global pandemic.
Although physical distancing is society’s main priority right now, this doesn’t change the fact that people still need routine and emergency medical care. For those suffering from a heart attack, stroke, or acute injury, the ER should still be the first destination. For regular medical visits, however, many providers are now offering their services remotely, so that they can still offer care to patients without asking the patients to put themselves or others at risk by traveling to a clinic, hospital, or private practice office. COVID symptom screenings can be done remotely, too, so that people can be advised by healthcare professionals about where to go for testing and care.
Also, the increase in telemedicine utilization isn’t limited to just internists! It often applies to specialties like mental health care and nutrition counseling, too. What’s more, both private insurance companies and programs like Medicare have loosened their restrictions on telehealth visits to facilitate providing care at a distance.
Overall, healthcare professionals and researchers are showing incredible ingenuity and dedication as they persevere in learning about, treating, and finding a vaccine for this devastating disease. Even those of us who aren’t on the front lines can do our part by following the guidelines put in place by public health officials and adhering to stay-at-home orders.
Want to learn more about the immune system and respiratory pathologies? Check out these related VB Blog posts:
- Anatomy and Physiology of the Lower Respiratory System
- The Lymphatic System: Innate and Adaptive Immunity
- Exploring Lung Pathologies with Physiology & Pathology
- VB News Desk: The Double Danger of Measles
- VB News Desk: Facts about the Flu
Be sure to subscribe to the Visible Body Blog for more anatomy awesomeness!
Are you an instructor? We have award-winning 3D products and resources for your anatomy and physiology course! Learn more here.



