Atherosclerosis: The Anatomy and Physiology of a (Silent) Killer
Posted on 9/1/17 by Marian Siljeholm
When I was six I tried to flush my stuffed animal cat down the toilet. Her name was Boots, and she was all black except for her white paws (hence the very creative name); she’d been my absolute favorite until she’d disappeared for three months. Ignoring the inherent chaos of moving several times that year, adolescent me was convinced that Boots had attempted to run away. I bring this up not to encourage an examination of potential irrational abandonment issues but rather for what happened to the pipes when they met Boots. (Spoiler alert: the story ends with a plumber and my losing allowance, playdates, and a whole host of other precious privileges for a small eternity.)
Pipe blockages can occur from large furry obstructions such as Boots, but arise more commonly from gradual buildups. As it turns out, the same is true for the human body and its "plumbing." In the case of humans, certain environmental and biological factors can cause fat, cholesterol, calcium, and other substances found in the blood to build up on artery walls, resulting in atherosclerosis. This narrowing of the vessels’ openings causes reduced blood flow and oxygen to cells, as well as a whole host of diseases and conditions your friendly neighborhood plumber certainly can’t fix.
Let’s take a look.
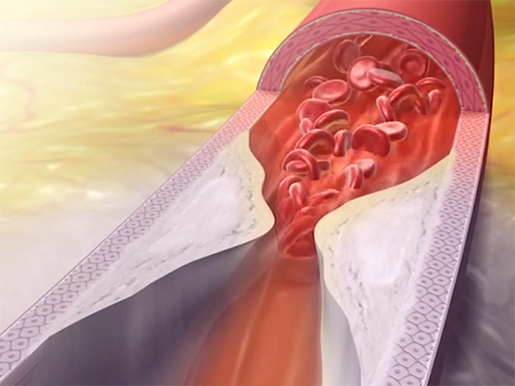 Image captured from Physiology Animations.
Image captured from Physiology Animations.
I’ll apologize in advance here for numerous anatomy 101 clarifications in this blog, but for the sake of clarity, I ask for patience from perusing healthcare professionals because this is a complex topic. As atherosclerosis is sometimes confused with cardiovascular disease (CVD), a term referring to a class of diseases that involves the heart or blood vessels, it’s worth differentiating that the term atherosclerosis refers solely to the hardening and narrowing of the arteries. Technically, atherosclerosis won’t kill you, but it’s the central contributor to many types of CVD that can.
It’s also worth differentiating between arteriosclerosis and atherosclerosis. Arteriosclerosis refers to the stiffening or hardening of the artery walls while atherosclerosis is the narrowing of the artery due to plaque buildup, rendering atherosclerosis a specific type of arteriosclerosis. Another relevant differentiation is that of arteries, which carry blood away from the heart; capillaries that exchange nutrients, waste, and oxygen with tissues at a cellular level; and veins, which bring blood back to the heart. Only arteries are susceptible to atherosclerosis. While the type of artery affected and where the plaque develops varies, once it develops, one of two scenarios is possible: either plaque breaks off and is carried by the bloodstream until it gets stuck, or a blood clot (thrombus) forms on the plaque’s surface. In both instances the artery can be blocked, cutting off blood flow and oxygen and resulting in several diseases, including:
- Coronary heart disease: Here plaque builds in arteries in or leading to the heart, which if undetected, eventually can lead to a heart attack.
- Carotid artery disease: Characterized by plaque in neck arteries that supply blood to the brain, CAD can often lead to a stroke.
- Peripheral artery disease (PAD): Here plaque builds in arteries of the extremities, especially the legs, which often causes pain, stiffness, and immobility. While this might appear less immediately lethal in comparison to the aforementioned stroke and heart attack, blockages in the extremities can travel, proving equally deadly to those originating near the heart or brain. Furthermore, if an artery supplying oxygen to the extremities (often the legs) is blocked and left untreated, gangrene (also known as tissue death) can result, which is very serious.
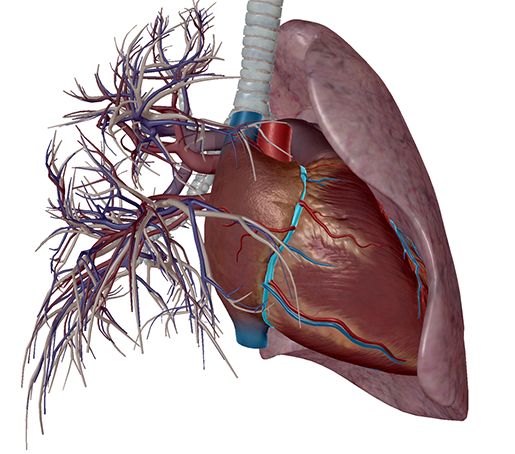
Highlighted in light blue is the right coronary artery. Image from Human Anatomy Atlas.
Presenting in some as early as adolescence, and in others not until after middle age, atherosclerosis is a slow, progressive condition, the symptoms of which can be subtle if present at all. As such, preventative treatment is aimed at preventing initial damage to arteries’ smooth interior surface (the endothelium), as this is responsible for initiating the lethal buildup.
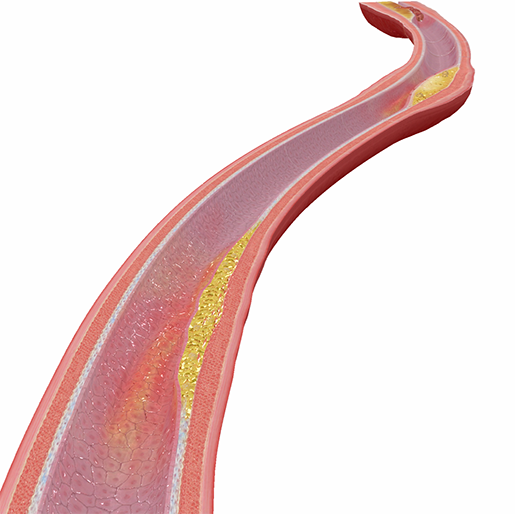 Plaque buildup and damage to endothelial cells in atherosclerosis. Image from Physiology & Pathology.
Plaque buildup and damage to endothelial cells in atherosclerosis. Image from Physiology & Pathology.
In addition to being obese, having diabetes or a family history of atherosclerosis, other risk factors include:
- High levels of LDL cholesterol: Also known as “bad cholesterol” for the way it crosses the damaged endothelium to form plaque on the artery wall, in response to which the body sends white blood cells to clean up the toxic site. Over years, continuing buildup of cholesterol coupled with this biological response create a plaque that hardens.
- High blood pressure: Elevated blood pressure puts stress on artery walls, rendering plaque more likely to break off, causing a heart attack or stroke. While high blood pressure can be caused by a genetic or preexisting condition, it’s often caused and exacerbated by decisions related to diet and exercise.
- Cigarette smoking: A terrible habit for numerous health-related reasons, smoking increases the likelihood of fatty deposits not only forming but also growing, which correlates heavily with both the early onset and rapid progression of atherosclerosis.
Check out more Anatomy & Physiology videos on our YouTube page.
Okay, so you’ve got plaque—what’s next? Given that the medical jury is still somewhat out regarding genetic causes of atherosclerosis, the bulk of treatment is bound to lifestyle changes, as well as medication and even surgery in more severe cases. The good news is none of the risk factors previously touched on is a sentence, even once the plaque has begun to build; by taking action you can help prevent or delay atherosclerosis and its related diseases through lifestyle changes, including:
- Diet: You are what you eat, and if you’re eating lots of things that create plaque such as high fat, cholesterol, and sodium foods, you’re likely to end up with plaque. Don’t shoot the messenger.
- Exercise! Physical activity (even 20 minutes a day, every little bit counts) keeps arteries healthy by lowering “bad” (LDL) cholesterol and boosting good cholesterol (spoiler alert, not all of it’s bad), in addition to reducing other risk factors such as high blood pressure, diabetes, obesity, and stress.
- Quit smoking! Seriously though. Quit. We aren’t saying it’s easy, but for this condition in particular it makes an enormous difference. Smoking has been shown to damage and tighten blood vessels and significantly raise your risk for atherosclerosis.
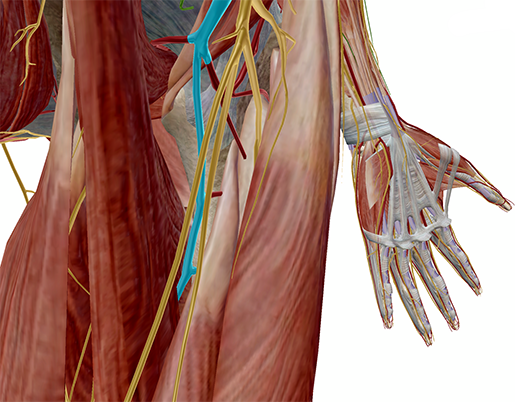 Highlighted in light blue is the profunda femoris (deep femoral) artery, from Human Anatomy Atlas.
Highlighted in light blue is the profunda femoris (deep femoral) artery, from Human Anatomy Atlas.
Given that symptoms usually don’t present until the disease is already in motion, don’t wait until you’re symptomatic if you present with any (or many) risk factors! Depending on the stage of plaque buildup, lifestyle changes might not be enough and medical intervention via cholesterol, anti-platelet, or other medication might be necessary. In more serious cases involving an advanced case or a blockage that threatens muscle or skin tissue survival, you may even need surgery. Needles, blood, and scalpels—oh my. (No thanks.)
I opened this with a lighthearted anecdote, however I’d do the repercussions of this condition a disservice if I didn’t ensure to impart the severity of its reality given the diseases it causes, as they result in hundreds of thousands of deaths annually in the United States alone. So, eat your veggies, take the stairs, and for goodness sake, don’t smoke! (Imploring for a fuzzy, once sodden best friend.)
Be sure to subscribe to the Visible Body Blog for more anatomy awesomeness!
Are you a professor (or know someone who is)? We have awesome visuals and resources for your anatomy and physiology course! Learn more here.
Related Posts:
Additional Sources:
“Disease Statistics.” National Heart Lung and Blood Institute, U.S. Department of Health and Human Services



