What We Know—And Don’t Know—About Long COVID
Posted on 12/17/21 by Sarah Boudreau
Some experts have called it “our next national health disaster.”
For almost two years, much of the medical research community has focused on COVID-19, and we have learned a lot since the initial lockdowns swept the globe. However, there is much we still don’t know about the lingering effects of COVID infections.
These long-term symptoms are called long COVID, long-haul COVID, or, if we are going to be more official, post-acute sequelae of SARS-COV-2 infection (PASC for short). A significant number of people who have contracted COVID experience long COVID; using data from April to December 2020, the UK Office for National Statistics reported that 22.1% of COVID patients experienced symptoms after five weeks and 9.9% had symptoms after 12 weeks.
In this blog post, we’ll talk about what long COVID is and what experts are doing to address it.
What exactly is long COVID?
As Dr. Lekshmi Santhosh, founder and medical director of the COVID OPTIMAL Clinic at the University of California, San Francisco, put it, “There is no one single long-COVID experience."
Broadly speaking, long COVID is when you experience symptoms for four or more weeks after acute infection. Long COVID can happen even when you have a mild case that does not require hospitalization.
The World Health Organization defines long COVID as such:
“Post COVID-19 condition occurs in individuals with a history of probable or confirmed SARS CoV-2 infection, usually 3 months from the onset of COVID-19 with symptoms and that last for at least 2 months and cannot be explained by an alternative diagnosis. Common symptoms include fatigue, shortness of breath, cognitive dysfunction but also others and generally have an impact on everyday functioning. Symptoms may be new onset following initial recovery from an acute COVID-19 episode or persist from the initial illness. Symptoms may also fluctuate or relapse over time.”
Symptoms
Many different symptoms fall under the umbrella of long COVID, which means that there is no way to test for it.
List of symptoms sourced from the CDC.
That’s an extensive list! Let’s unpack some of the common symptoms and explain them in further detail.
Fatigue is the most frequently reported symptom of long COVID. But why do many people experience fatigue after their acute COVID infection?
There are several possible causes:
- COVID might damage olfactory neurons, which reduces the outflow of cerebrospinal fluid through the cribriform plate. This could cause congestion in the glymphatic system, the system of perivascular channels that eliminate potentially neurotoxic waste from the brain.
- Inflammation and cell mediated immune mechanisms might cause hypometabolism in the frontal lobe and cerebellum, and this might last beyond initial COVID infection.
- Fatigue might be caused by psychological factors stemming from quarantine, illness, and the pandemic at large.
- The virus could infect and degrade skeletal muscle.
- A combination of the above!
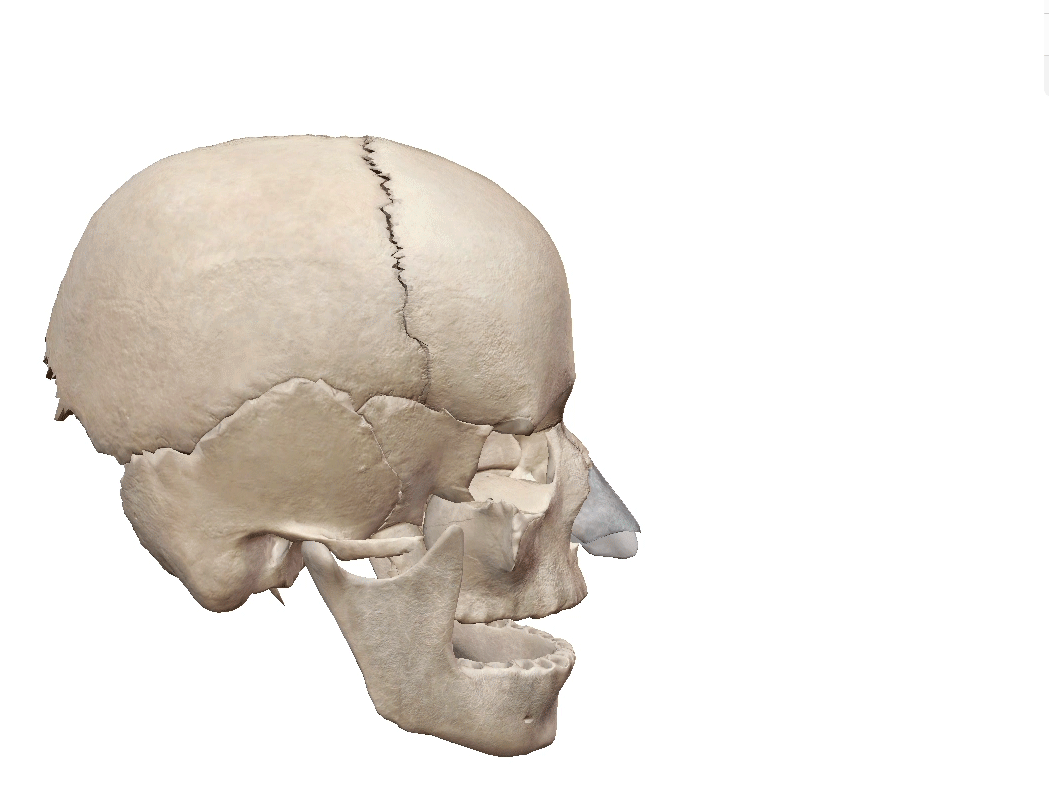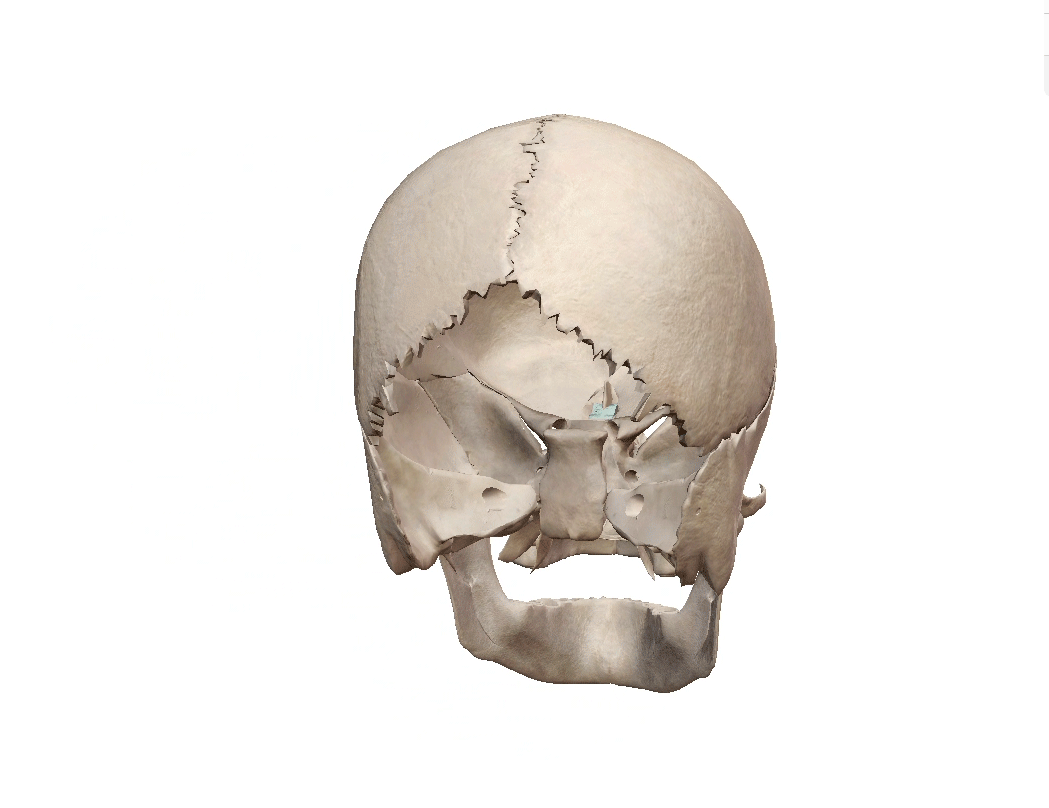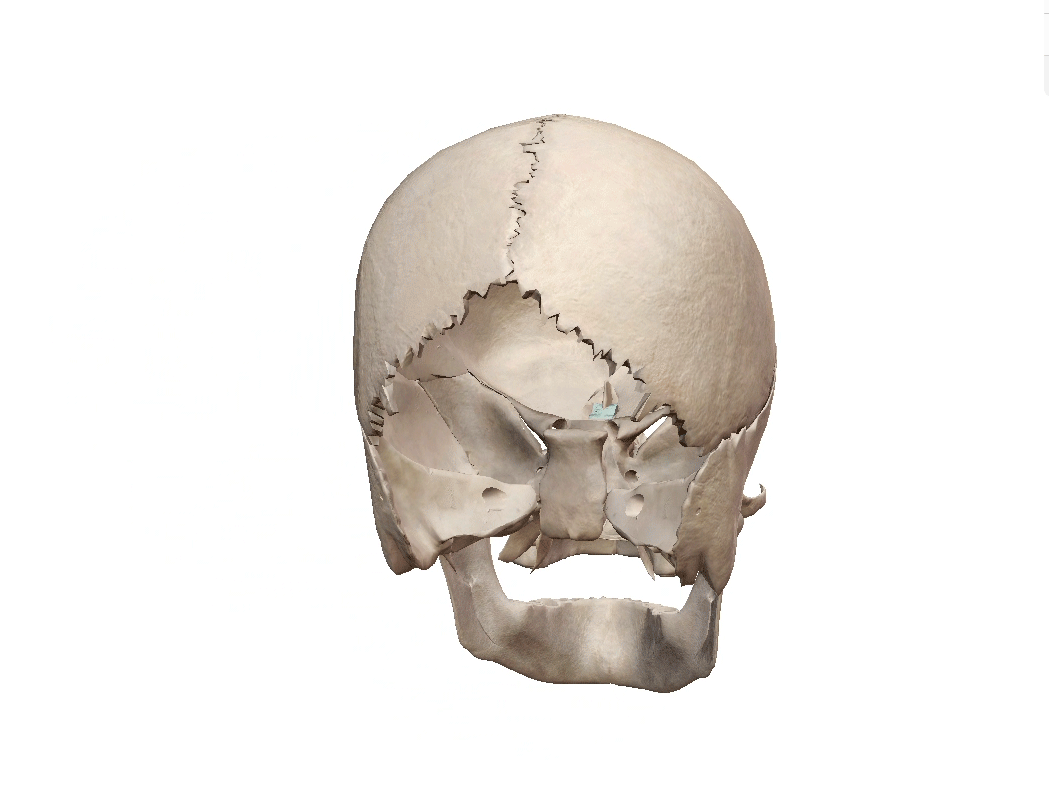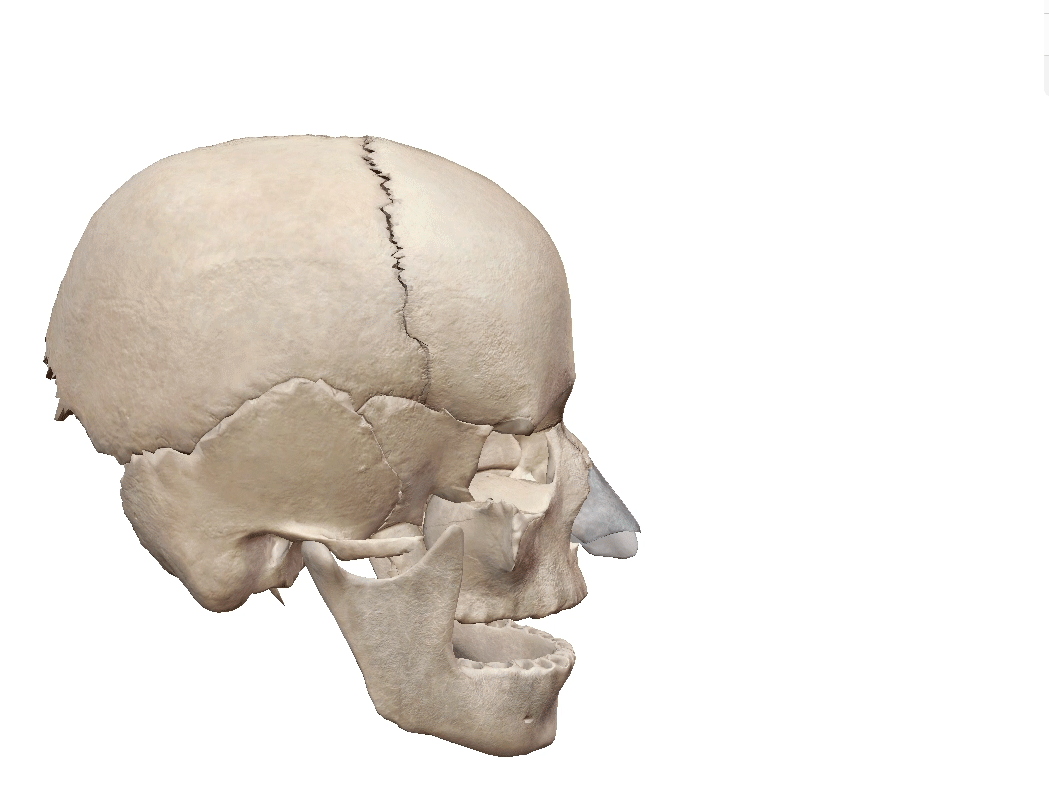
Cribriform plate (highlighted). GIF from Human Anatomy Atlas.
Shortness of breath is another particularly common lasting symptom for obvious reasons, as COVID is a respiratory illness. Most long COVID patients who experience shortness of breath were already at high risk of breathing difficulties when they contracted the virus, but COVID can also cause endothelial damage. This could create inflammation and interfere with the functioning of pulmonary endothelial cells, which account for a third of the cells in the lungs.
 Pulmonary ventilation (breathing) GIF from Physiology & Pathology.
Pulmonary ventilation (breathing) GIF from Physiology & Pathology.
Cognitive impairment is another common symptom of long COVID. Many different neurological symptoms are associated with COVID, with reports of hypoxic brain injuries, altered mental status, dysexecutive syndrome, and more. Approximately two thirds of ICU patients will experience delirium after their treatment—and that number is higher for people who have been on ventilators—but cognitive impairment has been reported in many long COVID patients who never went to the ICU. Many report “brain fog” that makes day-to-day tasks difficult, drawing comparisons to “chemo brain.”
Within the sphere of mental health, some of those who recover from COVID infections have reported post-traumatic stress disorder, depression, anxiety, and obsessive-compulsive symptoms. Social isolation can take a major toll on mental health, particularly for elderly people.
The symptoms of long COVID span all organ systems. Broadly speaking, scientists have identified several situations that could give rise to long COVID: the virus stays in the body to create these symptoms, it creates an inflammatory reaction that does not let up, or it creates autoimmune issues that cause these symptoms.
What’s being done to address long COVID?
2021 has seen the opening of more and more treatment centers specializing in long COVID.
The Survivor Corps, an organization that connects and supports COVID survivors, has recorded post-COVID care centers in 48 states and dozens of centers internationally.
In these centers, teams of professionals like pulmonologists, cardiologists, occupational and physical therapists, and behavioral health experts take a multidisciplinary approach to treating the wide variety of long COVID symptoms. Long COVID tends to take three to six months to resolve, though some cases can take a year or more.
 Photo from Shutterstock.
Photo from Shutterstock.
It’s important to underscore that we are still in the process of figuring out long COVID. We are still trying to figure out answers to seemingly simple questions like “Does vaccination decrease the risk of long COVID?”
An article in Nature points out the difficulties of finding a concrete answer to this question. A study of 1.2 million people through the COVID Symptom Study App developed by King’s College London and data-science company ZOE found that the risk of long COVID after a breakthrough infection was reduced, but as the Nature article points out, that study had its flaws. It had more women participants than men and fewer people from low-income areas, and it also left out brain fog and short-term memory loss as symptoms. Researchers are hard at work trying to understand more.
In February 2021, the National Institutes of Health announced the RECOVER Initiative, dedicated to supporting long COVID research.
Through funding research, the initiative seeks to answer questions like “What is the underlying biological cause of these prolonged symptoms?”, “How many people continue to have symptoms of COVID-19, or even develop new symptoms, after acute SARS-CoV-2 infection?” and “What makes some people vulnerable to this but not others?” In the fall, the NIH awarded about $470 million total to more than 100 researchers through this initiative.
Conclusion
Long COVID, described as symptoms four or more weeks after initial COVID infection, affects about a fifth of COVID patients. The symptoms are wide ranging in type and severity, and they sometimes require a personalized, multidisciplinary treatment plan.
More research is necessary before we can get to the bottom of long COVID and its effects on the millions of people who experience symptoms after their acute COVID infections.
Read more:
“Long-Haulers Are Fighting for Their Future” by Ed Yong in The Atlantic
“Characterizing long COVID in an international cohort: 7 months of symptoms and their impact” in EClinicalMedicine
“Cognitive Rehab: One Patient’s Painstaking Path Through Long Covid Therapy” by Pam Belluck in The New York Times
Learn about the Patient-Led Research Collaborative
Be sure to subscribe to the Visible Body Blog for more anatomy awesomeness!
Are you an instructor? We have award-winning 3D products and resources for your anatomy and physiology course! Learn more here.



